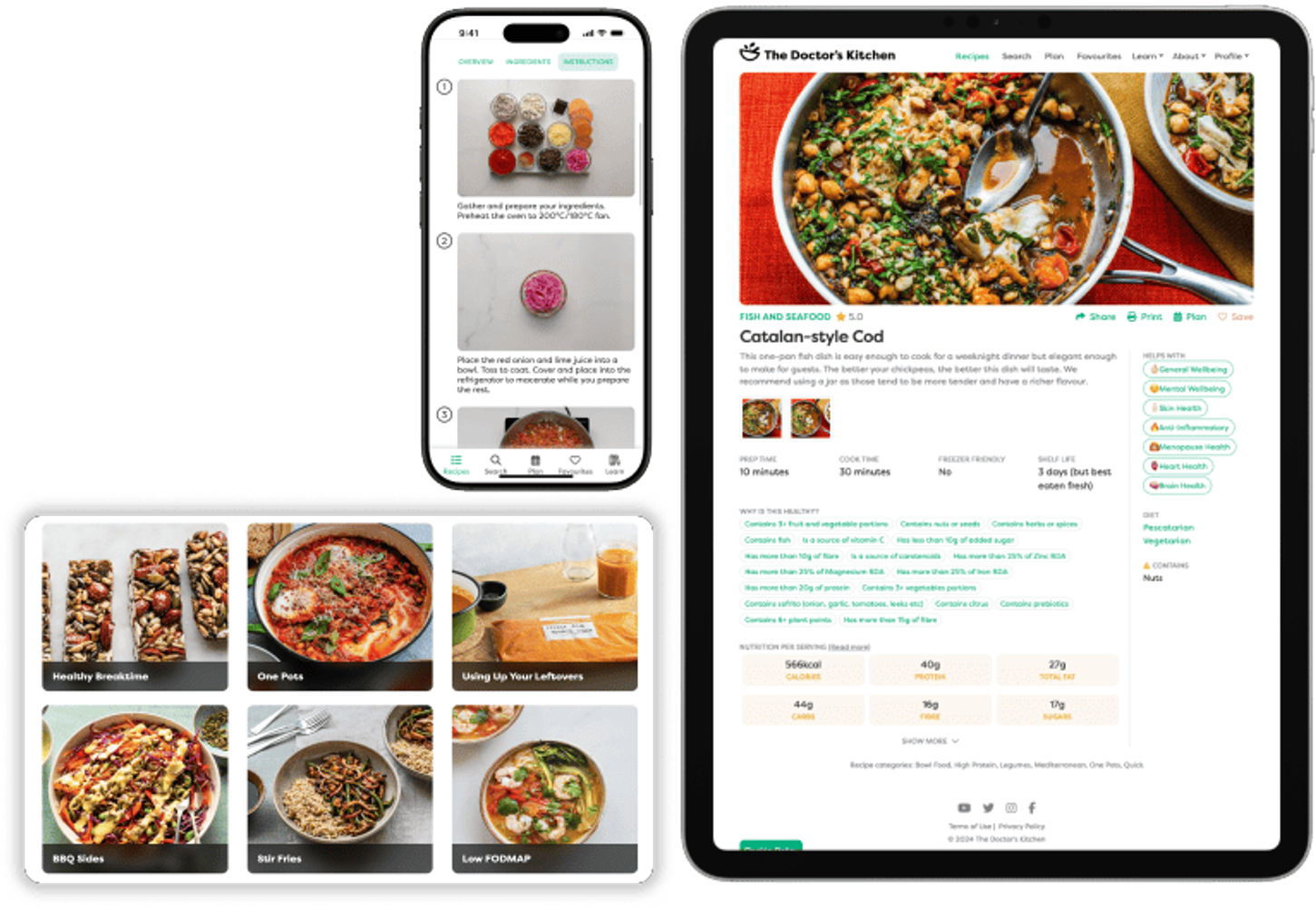
Polycystic Ovary Syndrome
28th Aug 2020
Everything you need to know about Polycystic Ovary Syndrome in one article...
Key points
WHAT IS POLYCYSTIC OVARY SYNDROME (PCOS)?
Polycystic ovary syndrome (PCOS) is a relatively common condition that affects the functioning of a woman’s ovaries. Although we do not know why some people get PCOS, it does appear to run in families. Approximately one in five women have the condition, but less than half will have symptoms.
There has been research using animal models to try to understand why PCOS might occur. One group have used a rat model, where they fed one group of pre-pubertal female rates a high fat diet, and the other identical group a normal diet. The high fat diet produced both the metabolic disturbances and ovarian changes similar to that observed clinically in PCOS patients. While this is interesting, more research needs to be undertaken to understand the mechanism of action of a high fat diet on the ovaries, and also if this is relevant to humans (1).
WHAT ARE THE SYMPTOMS OF PCOS?
Symptoms of PCOS include:
- Irregular or absent periods
- Excessive hair growth usually on the face, chest, back and buttocks called hirsutism.
- Weight gain
- Oily skin or acne
- Hair loss or thinning hair on the head
- Difficulty getting pregnant due to failure to ovulate or irregular ovulation
For more information see the NHS website.
WHAT IS INSULIN?
Insulin is an important hormone in our body, produced by the pancreas, that has a key role in controlling our blood sugar levels. When we eat, food is broken down and absorbed, leading to a rise in our blood sugar. The role of insulin is to signal to the muscles, fat and liver cells, to increase uptake of sugar from the bloodstream and store it. Insulin reduces the blood sugar level and keeps it within a tight range.
People with Type 1 diabetes stop producing insulin altogether, and so have to replace it with insulin injections when they eat, to keep their blood sugar levels within range. People with type 2 diabetes still produce insulin, but their cells become resistant to the signals from insulin, and so need higher levels of the hormone to respond. Type 2 diabetes is usually associated with being overweight. People with type 2 diabetes can sometimes control their sugar levels with weight loss through diet alone, but others will still need to take medication which increases the sensitivity of their cells to insulin signals.
WHY DOES INSULIN MATTER IN PCOS
Women with PCOS, have insulin resistance regardless of their weight, but the greater their weight, the greater the degree of insulin resistance and risk of type 2 diabetes. The majority of women with PCOS are more likely to be overweight. Diet is important in PCOS to ensure a healthy weight and to reduce the degree of insulin resistance. Women with PCOS have an increased risk of developing type 2 diabetes, high cholesterol and certain cancers. Those women with PCOS who are overweight also have a higher risk of infertility, hirsutism, spontaneous miscarriage, endometrial cancers and gestational diabetes (2). The good news is that even a modest weight loss of 5% of total body weight, can reduce these risks (2).
The NHS have a body mass index (BMI) calculator that you can use to see if you are a healthy weight.
PCOS TREATMENTS
The Oral Contraceptive Pill and PCOS (OCP) is often used in women with PCOS to protect the uterine lining, reduce androgenic symptoms such as hirsutism in addition to contraception. However, there is concern that it might not help insulin resistance and the disordered cholesterol profile commonly seen in women with PCOS. Additionally, the OCP can be associated with weight gain, which may further increase long term risk factors for cardiovascular disease.
There are a number of lifestyle changes that can improve symptoms, reduce future risk of disease and increase fertility.
WHAT SHOULD YOUR DIET LOOK LIKE WITH PCOS?
In general, if you have PCOS then think of your diet in the following ways:
Quality Fats
Aim for healthy unsaturated fats such as extra virgin olive oil, avocado, seeds, whole nuts, and rapeseed oil instead of saturated fats like those from coconut oil, butter and fatty meat (3). These types of unsaturated fats have been associated with improved glycaemic control and reduced insulin, that may play a role in PCOS symptom management and reduced risk of disease.
Quality Protein
In addition to trying to eat more quality fats and less unsaturated animal fats, there is evidence that replacing animal protein sources with plant based is beneficial too. In one study, two groups of women had the same diet, except one group had half the amount of animal based food, and instead had soya such as tofu. In the group that had less animal products and soy, glycaemic control, testosterone levels and cholesterol profiles improved (4). Similarly, women with PCOS who took soy isoflavone supplements (50m/day) had improved glycaemic control, hormonal status, and cholesterol profile (5). For more information about the nuanced topic of isoflavone supplements and breast cancer I would suggest reading this article.
Trans Fats
Trans fats, from fried foods, ready meals, shop bought pastries and high heat degradation of fats, have been associated with a failure to ovulate, and other general health concerns such as increased cancer risk, so it is best to minimise or remove these foods if possible. Diets low in trans fats and high in fibre have also been associated with increased glucose tolerance, and improved cholesterol profile in women with PCOS (6).
Eat Regularly and Curb Snacking
There has been research that found that those people who ate irregularly were more likely to eat a higher fat, protein, cholesterol and salt diet. While those who ate regularly were more likely to have a more balanced diet, with higher carbohydrate and fibre levels, with more micronutrients. Additionally, those who ate regularly were more likely to have a better glucose profile, with less insulin resistance, so it is likely that eating regular meals and curbing snacking would also benefit women with PCOS.
Potential for Low Carbohydrate Diet
Short term (meaning for less than 6 months) restriction of carbohydrates can kick start weight loss and improve cardiovascular risk. However, evidence to support long term use is lacking (7,8). Recent data from a large study has found that low carbohydrate diets (<40% daily energy from carbohydrates), where carbohydrates are substituted with animal fat were associated with a higher risk of early death (9). However, for those people who substituted carbohydrates with plant-based fat and protein, they had a lower mortality and cardiovascular risk (9).
Low carbohydrate diets have been associated with better short term control of blood sugar in type 2 diabetes, but there is insufficient evidence of long term benefit (8,10). In PCOS, restriction of carbohydrates may improve insulin resistance, but more research is needed to see if this is the case, and if there is any long-term benefit.
Calorie Restriction
Reduction of fat, protein and carbohydrate to create an energy deficit and increasing your exercise regimen are an alternative option to reduction in just carbohydrates. When starting a calorie restriction diet, aim to eat about 200 kcal less than you need each day. After a couple of weeks, you can slowly move this to 500 kcal less than you need each day. When undertaking calorie restriction diets it is best practice to consult a registered practitioner such as a dietician or nutritionist.
Gut Health
The micro-organisms that live in your gut (microbiota) have also been shown to play a role in PCOS. The gut microbiota can lead to chronic inflammation, metabolic syndrome, insulin resistance and hyperandrogenism (high testosterone) (11). Women with low biodiversity have higher testosterone and hirsutism (12). Diets high in fibre, and low in trans fats as mentioned above, have been associated with increased glucose tolerance, and improved cholesterol profile in women with PCOS (6).
Additionally, probiotic supplements have been found to improve a number of symptoms (see below). A blinded, randomised controlled trial that divided women with PCOS into 3 matched groups, where they received pomegranate juice, a synbiotic (mixture of pre and probiotics) drink, and a synbiotic pomegranate juice, found that drinking the synbiotic drink or synbiotic pomegranate drink was associated with improved glucose tolerance, insulin profiles, decreased testosterone, BMI, weight and waist circumference (13).
There is some suggestion that a disrupted gut-brain axis, could explain the co-occurrence of increased mood disorders along with obesity and abnormal appetite in PCOS (14). So supporting your gut microbiota with prebiotic foods (for example chicory, lentils, leeks, apples, barley) and natural probiotics such as fermented foods (kefir, kimchi, tempeh), may help improve your PCOS.

OVULATION IN PCOS
Ovulation is dependent on a number of hormones which all rise and fall at different times within the menstrual cycle. A surge of the hormone Luteinising Hormone (LH) is necessary for a mature ovum to be released at ovulation. LH is the hormone detected by ovulation test kits. In PCOS, insulin resistance, leads to increased androgen hormones, and suppresses Luteinising hormone (LH), which is needed for ovulation. This means that many women with PCOS either ovulate infrequently, or not at all, leading to irregular periods and difficulty conceiving. Short term calorie restriction resulting in weight loss, has been shown to reduce levels of the androgen hormones, which restores the normal LH surges and therefore ovulation cycles (2).
WHY DO I GET CARBOHYDRATE CRAVINGS?
Women with PCOS are more likely to have insulin and blood sugar levels that fluctuate more. This has been associated with a reactive low blood sugar after meals, leading to carbohydrate cravings, a frequently reported symptom for women with PCOS.
WHAT IS THE GLYCAEMIC INDEX AND WHY DO I NEED TO KNOW?
Glycaemic index (GI) is a ranking of carbohydrates based on how quickly they are broken down, absorbed and affect the sugar levels in the blood. Low GI foods are broken down slowly, such as brown rice, broccoli and wholegrain pasta. Whereas high GI foods rapidly affect blood sugar levels, such as sugar, pineapple and chocolate. Aim to eat lower GI foods where possible.
For more information on Glycaemic Index please have a look at this page on the NHS website.
EXERCISE AND PCOS
Surprisingly very little research has been done on the role of exercise in women with PCOS. At present approximately 30 minutes of exercise on at least 5 days of the week is generally recommended to maintain a static weight. To promote weight loss, 60-75 minutes 5 times per week of moderate to high intensity exercise is needed. However, any exercise is better than none, and a good place to start to get up to the recommended amounts.
Physical exercise in women with PCOS has been shown to be associated with the following benefits (15):
- Improved menstrual regularity
- Increased ovulation rates
- Increased chance of pregnancy
- Improved lipid profiles
- Decreased waist circumference
- Lower systolic blood pressure
- Reduced fasting insulin
More research is needed to determine the optimum Intensity, duration and type of exercise. Also further understanding to determine if it is exercise that is directly having a benefit in PCOS or any associated weight loss.
SUPPLEMENTS
Women with PCOS and vitamin D deficiency have been found to have a higher likelihood of insulin resistance and fasting glucose levels (16). A systemic review, looked at the evidence of improvement of these measures with supplementation of vitamin D. Eleven randomised controlled trials totalling 600 women, were analysed together, and demonstrated that supplementation improved insulin resistance and fasting glucose levels (17). Therefore, it is important to ensure you have sufficient vitamin D levels.
One double blinded, placebo-controlled trial found that the combination of vitamin D and probiotics for 12 weeks improved testosterone levels, hirsutism, markers of inflammation and had a beneficial effect on mental health (18).
Zinc supplements (50mg/day) have been found to improve hair loss and hirsutism, but did not affect hormonal profiles (19). Coenzyme Q10 (100mg/day) for 12 weeks was found to improve glucose metabolism and cholesterol profiles (20). Combined supplementation of zinc (4mg/day), vitamin D (200IU/day), with calcium (400mg/day) and magnesium (100mg/day) have been found to have a beneficial effect on some hormone profiles and markers of inflammation (21). There isn’t good research to know if having a diet which is rich in zinc, calcium and magnesium has the same effects.
Other supplements such as chromium (22) have been trialled in PCOS, but not shown to have a significant benefit (23).
Evidence from a systemic review that included 3 randomised controlled trials, totalling 140 women, did not find any improvement in fasting glucose or insulin resistance (24) with supplementation of omega 3.

SUMMARY
While it isn’t possible to cure PCOS there are a number of lifestyle changes that can reduce your symptoms, long term risk of cardiovascular disease, and increase your fertility:
- Swap refined carbohydrates (white bread, white pasta, and sugary items) for whole grains (brown rice, wholegrain bread, wholegrain pasta, millet and bulgur wheat)
- Aim to eat lots of fruit, vegetables which are high fibre and full or antioxidants such as leafy greens (spinach, chicory), cruciferous (cauliflower, cabbage, broccoli including the stem), marrows (courgettes, squash), roots (carrots, sweet potatoes), allium (onions, garlic, leeks) and edible stems such as asparagus
- Eat more whole grains, lean protein (poultry, fish), soy (tofu, tempeh) and more unsaturated fat such as extra virgin olive, flaxseed, rapeseed oils and avocado
- Consider reducing your carbohydrate intake, and substituting for plant-based fats not animal fats
- Try replacing meat with plant based foods such as lentils, beans, tofu, tempeh and tofu
- Drink unsweetened drinks such as water
- Avoid trans fats often found in shop bought baked goods and ready meals
- Support your microbiome with lots of fruit and vegetables (see above), fermented products such as kefir, kimchi, and raw fermented vegetable slaw. Consider taking a probiotic
- Try to avoid snacking, instead choose a regular pattern of meals
- Ensure your vitamin D level is sufficient (supplement during the autumn and winter months, and safe sun exposure) and consider supplementing zinc, magnesium, calcium and coenzyme Q10
- A minimum of 30 minutes of exercise 5 times per week

Article Credit: Dr Harriet Holme (https://healthyeatingdr.com/)
REFERENCES
- Patel R, Shah G. High-fat diet exposure from pre-pubertal age induces polycystic ovary syndrome (PCOS) in rats. Reproduction. 2018 Feb;155(2):141–51.
- Farshchi H, Rane A, Love A, Kennedy RL. Diet and nutrition in polycystic ovary syndrome (PCOS): pointers for nutritional management. J Obstet Gynaecol. 2007 Nov;27(8):762–73.
- Moran LJ, Grieger JA, Mishra GD, Teede HJ. The Association of a Mediterranean-Style Diet Pattern with Polycystic Ovary Syndrome Status in a Community Cohort Study. Nutrients. 2015 Oct 16;7(10):8553–64.
- Karamali M, Kashanian M, Alaeinasab S, Asemi Z. The effect of dietary soy intake on weight loss, glycaemic control, lipid profiles and biomarkers of inflammation and oxidative stress in women with polycystic ovary syndrome: a randomised clinical trial. J Hum Nutr Diet. 2018 Aug;31(4):533–43.
- Jamilian M, Asemi Z. The Effects of Soy Isoflavones on Metabolic Status of Patients With Polycystic Ovary Syndrome. J Clin Endocrinol Metab. 2016 Sep;101(9):3386–94.
- Nybacka Å, Hellström PM, Hirschberg AL. Increased fibre and reduced trans fatty acid intake are primary predictors of metabolic improvement in overweight polycystic ovary syndrome-Substudy of randomized trial between diet, exercise and diet plus exercise for weight control. Clin Endocrinol (Oxf). 2017 Dec;87(6):680–8.
- Brouns F. Overweight and diabetes prevention: is a low-carbohydrate-high-fat diet recommendable? Eur J Nutr. 2018 Jun;57(4):1301–12.
- Snorgaard O, Poulsen GM, Andersen HK, Astrup A. Systematic review and meta-analysis of dietary carbohydrate restriction in patients with type 2 diabetes. BMJ Open Diabetes Res Care. 2017;5(1):e000354.
- Seidelmann SB, Claggett B, Cheng S, Henglin M, Shah A, Steffen LM, et al. Dietary carbohydrate intake and mortality: a prospective cohort study and meta-analysis. The Lancet Public Health. 2018 Sep 1;3(9):e419–28.
- Meng Y, Bai H, Wang S, Li Z, Wang Q, Chen L. Efficacy of low carbohydrate diet for type 2 diabetes mellitus management: A systematic review and meta-analysis of randomized controlled trials. 2017 Sep;131:124–31.
- Zhao X, Jiang Y, Xi H, Chen L, Feng X. Exploration of the Relationship Between Gut Microbiota and Polycystic Ovary Syndrome (PCOS): a Review. Geburtshilfe Frauenheilkd. 2020 Feb;80(2):161–71.
- Torres PJ, Siakowska M, Banaszewska B, Pawelczyk L, Duleba AJ, Kelley ST, et al. Gut Microbial Diversity in Women With Polycystic Ovary Syndrome Correlates With Hyperandrogenism. J Clin Endocrinol Metab. 2018 Apr 1;103(4):1502–11.
- Esmaeilinezhad Z, Babajafari S, Sohrabi Z, Eskandari M-H, Amooee S, Barati-Boldaji R. Effect of synbiotic pomegranate juice on glycemic, sex hormone profile and anthropometric indices in PCOS: A randomized, triple blind, controlled trial. Nutr Metab Cardiovasc Dis. 2019 Feb;29(2):201–8.
- Ilie IR. Neurotransmitter, neuropeptide and gut peptide profile in PCOS-pathways contributing to the pathophysiology, food intake and psychiatric manifestations of PCOS. Adv Clin Chem. 2020;96:85–135.
- Benham JL, Yamamoto JM, Friedenreich CM, Rabi DM, Sigal RJ. Role of exercise training in polycystic ovary syndrome: a systematic review and meta-analysis. Clin Obes. 2018 Aug;8(4):275–84.
- He C, Lin Z, Robb SW, Ezeamama AE. Serum Vitamin D Levels and Polycystic Ovary syndrome: A Systematic Review and Meta-Analysis. Nutrients. 2015 Jun 8;7(6):4555–77.
- Łagowska K, Bajerska J, Jamka M. The Role of Vitamin D Oral Supplementation in Insulin Resistance in Women with Polycystic Ovary Syndrome: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Nutrients. 2018 Nov 2;10(11):1637.
- Ostadmohammadi V, Jamilian M, Bahmani F, Asemi Z. Vitamin D and probiotic co-supplementation affects mental health, hormonal, inflammatory and oxidative stress parameters in women with polycystic ovary syndrome. J Ovarian Res. 2019 Jan 21;12(1):5–8.
- Jamilian M, Foroozanfard F, Bahmani F, Talaee R, Monavari M, Asemi Z. Effects of Zinc Supplementation on Endocrine Outcomes in Women with Polycystic Ovary Syndrome: a Randomized, Double-Blind, Placebo-Controlled Trial. Biol Trace Elem Res. 2016 Apr;170(2):271–8.
- Samimi M, Zarezade Mehrizi M, Foroozanfard F, Akbari H, Jamilian M, Ahmadi S, et al. The effects of coenzyme Q10 supplementation on glucose metabolism and lipid profiles in women with polycystic ovary syndrome: a randomized, double-blind, placebo-controlled trial. 2017 Apr;86(4):560–6.
- Maktabi M, Jamilian M, Asemi Z. Magnesium-Zinc-Calcium-Vitamin D Co-supplementation Improves Hormonal Profiles, Biomarkers of Inflammation and Oxidative Stress in Women with Polycystic Ovary Syndrome: a Randomized, Double-Blind, Placebo-Controlled Trial. Biol Trace Elem Res. 2018 Mar;182(1):21–8.
- Maleki V, Izadi A, Farsad-Naeimi A, Alizadeh M. Chromium supplementation does not improve weight loss or metabolic and hormonal variables in patients with polycystic ovary syndrome: A systematic review. Nutr Res. 2018 Aug;56:1–10.
- Arentz S, Smith CA, Abbott J, Bensoussan A. Nutritional supplements and herbal medicines for women with polycystic ovary syndrome; a systematic review and meta-analysis. BMC Complement Altern Med. 2017 Nov 25;17(1):500–14.
- Sadeghi A, Djafarian K, Mohammadi H, Shab-Bidar S. Effect of omega-3 fatty acids supplementation on insulin resistance in women with polycystic ovary syndrome: Meta-analysis of randomized controlled trials. Diabetes Metab Syndr. 2017 Jun;11(2):157–62.